Connecting state and local government leaders
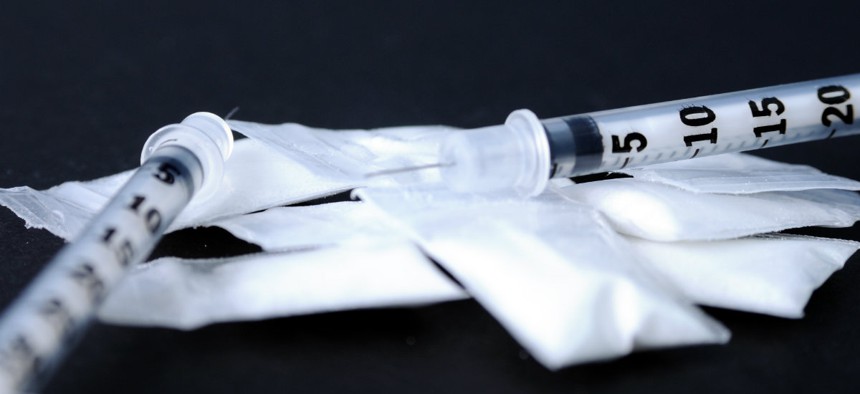
The state leads the nation in new diagnoses, and close to six percent are attributed to injection-drug users sharing used or infected needles.
On a steamy Tuesday, I sat in the passenger side of Emelina Martinez’s car as she wove through Overtown, a neighborhood in Miami notorious for opioid drug use, sales, and overdoses. Martinez, 48, is an outreach coordinator at IDEA Exchange, Florida’s first needle exchange that opened in Overtown in December. She drives through the neighborhood a few times each day, spreading the word and checking in on participants, the overwhelming majority of whom are intravenous drug users who call Overtown’s underpasses and parking lots home.
As we drive, Martinez spots a woman she doesn’t recognize and pulls over. “Baby,” she calls. She passes the woman a flyer and condoms. “In case you know somebody who injects,” she says, pointing at the flyer.
The woman nods. “My friend wanted to know about this.”
In 2015, Florida led all 50 U.S. states in new HIV diagnoses. The same year, Miami-Dade and Broward Counties averaged close to 40 new diagnoses per 100,000 people—three times the national average. Nationwide, the number of new HIV diagnoses has been on the decline—down 19 percent from 2005 to 2014.
As of December, the lion’s share of new infections in Miami-Dade came from unprotected sex. But close to six percent are attributed to injection drug users sharing used or infected needles—a number the staff at IDEA believes can be curbed, with support.
Although Florida leads the nation in new HIV infections, some argue this is not being treated as a crisis by Governor Rick Scott or the state Department of Health. Last year, Scott cut more than $30 million in funding and over 700 state and county jobs from Florida’s health department, though a spokesperson at the time told the Tampa Bay Times that “no department services or readiness capabilities will be interrupted.” Democrats in the Florida Senate recently urged Scott to declare the state’s opioid epidemic a public health emergency.
“It’s been a tough dance with the state,” said Hansel Tookes, a resident at Jackson Memorial Hospital. It took Tookes five years of lobbying and multiple appearances before the Florida legislature to get a bill signed approving IDEA to open under the guidance of the University of Miami. He considers it a win, but said it doesn’t change the fact the state is late to the party. “This is 1990s drug policy we just got after blood, sweat, and tears.”
As of 1998, at least 100 needle exchanges operated in 31 states. By 2014, there were 194 in 34 states. California, right behind Florida in new HIV infections in 2015, has over 40 exchanges according to the North American Syringe Exchange Network. Meanwhile, federal support has been finicky. In 2009, a ban on federal funds dating back to 1988 was lifted. It was then reinstated in 2011. In January 2016, it was lifted again—a decision that came on the heels of climbing intravenous drug use nationwide and an outbreak of HIV in rural Indiana.
With the latest ruling, federal funds cannot purchase needles but can be used to do things like pay staff, buy vehicles or other equipment, and help exchange sites refer users to treatment. To gain access to funds, exchanges as well as state and local health departments must provide evidence of need to the Centers for Disease Control and Prevention. As it stands, Florida prohibits IDEA from state, county, or municipal funds.
Tookes said Miami easily demonstrates need for federal aid and is hopeful that in the next year he can convince state and local officials to agree. But he isn’t holding his breath. “I’m constantly writing grant proposals,” he said. So far, IDEA has raised $700,000 from donors including the AIDS Healthcare Foundation, which also stepped in to provide free HIV and Hepatitis C testing kits when the county and state health departments refused, according to Tookes.
IDEA’s operation is small. A staff of three work out of two storage containers turned offices. An electricity line runs from the back of one and into a University of Miami storage facility behind them. IDEA has an address, but staff admit they’re technically located in a parking lot. Still, close to three months after opening, they’ve enrolled 156 participants—almost all of whom self-identify as intravenous drug users. They have tested roughly half for HIV and have collected 8,686 dirty needles off the streets in exchange for 7,594 clean ones.
Carlos Padron, 25, mans the front desk. During a lull one afternoon, he shows me an inventory of needles in various lengths and sizes—a 29-inch version is most popular. Next to the needles are boxes containing small packets of sterile water, aluminum cookers, condoms, rubber tourniquets, alcohol pads, and a canteen to store “dirties” until they can be exchanged. When participants visit and request items, he packs them in a brown paper bag.
Padron said a common misconception about exchanges is they give users the tools to get high. The problem, he believes, is most people don’t understand the nature of addiction. “They are going to use no matter what,” he said. He knows of one participant who reused a needle so many times he had to sharpen it on concrete in order to puncture his skin. “Why not give them clean needles and have somewhere they can come where they won’t be judged and they can get help?”
To be a participant, people must register in a database using anonymous initials. They are asked to identify basic demographic information about themselves—according to data provided by IDEA, over 70 percent of its participants are white males and on average, they are 38 years old—as well as what drugs they inject, how often, whether they’re infected with HIV or Hepatitis C, and if they’d like to be tested. Another section asks if they’d like help receiving treatment for HIV, Hepatitis C, or drug dependence. So far, 25 participants have been referred to either drug treatment centers or medically supervised HIV and Hepatitis C treatment.
After registering, they’re given a participant number and ID card that allows staff to track the number of needles they bring in and receive. IDEA is a one-for-one exchange, meaning participants receive as many needles as they trade in—although some visitors drop off needles without asking for any in return. More importantly for participants who live on the street, an ID protects them from being in violation of Florida’s Drug Abuse Prevention and Control Act if they’re stopped by police and have dirty needles.
In theory, at least.
While spending the day at IDEA, a participant identified by the initials R.L. walked in with one needle to exchange and no ID. R.L., 50, said he was arrested on Christmas Day and spent a month in prison after being found with needles and a few used bags of heroin. He had lost his ID before being arrested. “I’m homeless, so I have things here and there,” he explained.
Before the passage of the Infectious Disease Elimination Pilot Program in March, needles were classified as drug paraphernalia. However, with the authorization of the pilot, possession of needles—acquired from IDEA—no longer violates the law. R.L.’s baggies were grounds for arrest, but he illustrates the tricky entanglement IDEA, its participants, and law enforcement must navigate: Participants can walk around with needles for the purpose of drug use, but must not have drugs or evidence of drugs if stopped and must always have their ID card. Meanwhile, authorities must learn how to factor these new rules into their daily encounters.
“The law has been worked out on a higher administrative level, but that doesn’t mean it has been worked out on the street,” said Daniel Johnson, day to day director at IDEA. When I visited one afternoon, Johnson had wrapped up a meeting with two members of the local police force in Overtown to discuss the arrests of numerous participants. Johnson said he gave them a detailed explanation of how to spot participants and how the new law protects them. He said it was the first of two meetings he’s had with authorities since opening.
When asked about any adjustments local police have had to make in Overtown, Commander Nicole Davis declined to comment directly. She said IDEA was not specific to Overtown and that officers were enforcing narcotics and paraphernalia possession in accordance with state laws. Assistant State Attorney Howard Rosen declined to speak on behalf of law enforcement.
“They’re starting to come around, but they don’t always see the other side of the coin,” said Johnson, about IDEA’s relationship with authorities. He acknowledges the abrupt change in policy, but stressed that in order to encourage participants to be responsible with dirty needles, they must feel safe transporting them. “We can’t look at these folks from the lens of the law enforcement,” he said, “We have to look at them from a public health lens.”
Jose De Lemos, 54, said the trouble with that is society has a negative perception of intravenous drug users, a stronger stigma than that placed on users of substances like cocaine or alcohol. De Lemos, a frequent visitor to and volunteer at IDEA, is a man who embodies the sort of transformation staff hope to inspire. As a former heroin user for more than 10 years, he spent long stretches living in the streets of Overtown. In 2012, he was diagnosed with HIV after sharing a needle. Shortly after, he became a patient of Tookes.
As we spoke, he showed me an old photo of himself. His face was pockmarked with a severe rash that has now mostly cleared. Participants who remember De Lemos from the streets are often stunned to find him alive. He said it feels good knowing he gives them hope. “Right now, that’s one of the most important things we can give them.”
In the coming year, IDEA plans to launch a mobile unit to expand to other parts of South Florida. Tookes said he believes broadening the exchange’s reach and eventually helping similar efforts get off the ground in other counties, can also help fight the state’s dire epidemic of heroin and fentanyl use that emerged as an unfortunate side-effect of a crackdown on “pill mills.” In the first half of 2015, heroin deaths were up 215 percent in Broward County and 425 percent in Palm Beach County compared to the same period in 2014. Nationwide, heroin use is at a 20-year high.
“The state is reeling from these epidemics,” said Tookes over breakfast. “But there is still a disconnect between what is happening and what we’re doing.” He points to cities like New York and their push to distribute free condoms and advertise the preventative HIV medication PrEP on subways and in the streets, as the sort of proactive public-health interventions he’d like to see.
As we spoke, Tookes wore shades to hide dark bags under his eyes after an overnight shift at Jackson Memorial. In July, he starts a new position at the University of Miami and will play a more active role in the day to day work at IDEA while advocating for further legislation to expand public health solutions to address Florida’s HIV infections and opioid use. He looked out to Brickell Bay, illuminated by a gleaming sun. “I think, symbolically, a huge shift was getting the needle exchange. I think we’re on the right path,” he said.
Andrew Boryga is a writer based in South Florida. This article was originally published in The Atlantic.

NEXT STORY: Confronting the Challenges of Getting Timely Opioid Abuse Data