More Than 72,000 Lose Medicaid Coverage in Arkansas

An unprecedented nationwide review of the millions of Medicaid enrollees over the next year will require states to remove people whose incomes are now too high for the federal-state program. Jahi Chikwendiu/The Washington Post via Getty Images
Thousands of children lost coverage in the state's effort to update enrollment—a process taking place nationwide as states review the eligibility of millions of Medicaid enrollees following the public health emergency.
Arkansas removed more than 44,000 people, whose coverage had been extended because of the Covid-19 public health emergency, from the state’s Medicaid program at the end of April, the Department of Human Services announced Monday.
Another 28,135 cases were closed as part of the department’s normal operations, bringing the total number of disenrollments for the month to 72,802.
“That is pretty high,” said Jennifer Tolbert, associate director with KFF’s program on Medicaid and the uninsured, adding, “The one note of caution in all of this is that this is the first month. This is the only set of data. While it does raise red flags, we don’t know how this will play out.”
Nationwide, states are currently undertaking the herculean task of checking whether all of the nation’s roughly 93 million low-income people on Medicaid still qualify for coverage. States were barred from dropping people’s coverage during the pandemic, but that’s ended now. Congress discontinued the restriction in the $1.7 trillion omnibus spending bill it passed in December, allowing states to remove those who do not qualify from the rolls on April 1. States have 14 months to make sure everyone in the program is eligible.
As reported last month, states’ timelines to make those decisions vary. Most states report that they plan to take between a year and the full 14 months allowed to complete the effort, according to a survey of state Medicaid agencies conducted in January by KFF and Georgetown University’s Center for Children and Families. Five states—Arkansas, Montana, New Hampshire, Oklahoma and South Dakota—are planning to finish in as little as nine months. But Arkansas’ legislature directed its state Medicaid office to cull the list within six months, or about twice as quickly as most states.
Monday’s report is the first month of data since the so-called unwinding process—reviewing recipients’ eligibility—began. But some of the initial numbers in the report are raising red flags for observers.
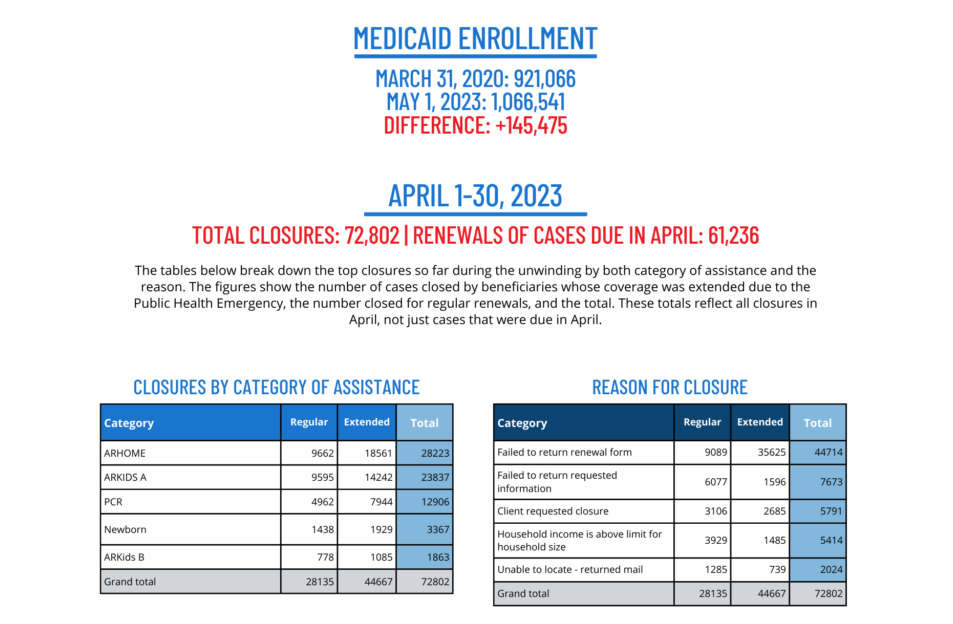
Most notably, the data the state released reveals that more than 29,000 children in the state lost their Medicaid coverage in April—17,256 of which were beneficiaries whose coverage was extended due to the public health emergency (PHE). In other words, 40% of the recipients losing coverage are kids, according to Joan Alker, executive director of the Center for Children and Families and a research professor at the Georgetown McCourt School of Public Policy.
The Center for Children and Families released a report in February warning that uninsured rates for children could rise sharply during the unwinding process if states aren’t careful. “The vast majority of children (73.6%) losing coverage will remain eligible for Medicaid but are likely to lose coverage due to bureaucratic snafus,” the report said. “The uninsured rate for children could easily more than double if states have inadequate staffing levels and overwhelmed call centers and do not take the time and care needed to properly conduct eligibility checks after the federal protections lift.”
Alker said that the 40% disenrollment of children was “very big” and called on Arkansas Gov. Sarah Huckabee Sanders to “...PAUSE Medicaid terminations at least for children (preferably adults too) to assess what’s going wrong.”
Another red flag, according to Tolbert, is the high percentage of people disenrolled for procedural reasons.
Citing numbers that Arkansas submitted to the Centers for Medicare & Medicaid Services, which were slightly different from the press release the state issued yesterday, the majority—about 90%— were removed for not providing the required information to determine their eligibility or because the state was unable to locate them.
“It is somewhat concerning,” she said. “But again, this process is happening quickly and we don’t know how many times the state reached out and how much time they allowed for people to respond. When you are trying to complete a process in six months, that suggests that there is not time to reach out and allow time to respond.”
In its press release, the department said it “is moving swiftly to disenroll individuals who are no longer eligible to ensure that Medicaid resources go to beneficiaries who truly need them, and this will continue in the coming months as the unwinding progresses.”
Last month, Bradley Corallo, also a senior policy analyst with KFF’s program on Medicaid and the uninsured, told Route Fifty that about 15 million people are expected to lose their Medicaid coverage, according to an estimate by the U.S. Department of Health and Human Services. But most concerning is that, according to the estimate, about 6.8 million of those who will lose coverage are expected to be wrongly booted from Medicaid even though they qualify for the program.
Another concern that Corallo cited is how well states will be able to reach people to let them know they have to reenroll.
To those concerns in light of Arkansas’ report, Tolbert said, “We need one or two more data points to assess if the process is working or not.”





