How governments are tackling medical debt
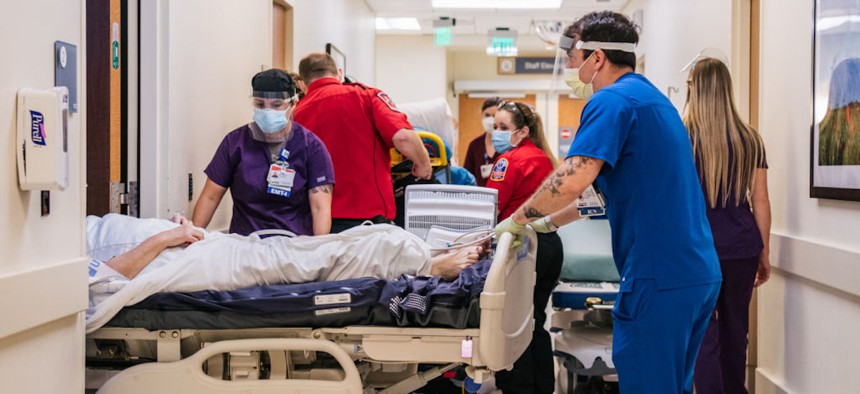
Emergency Room nurses and EMTs tend to patients in hallways at the Houston Methodist The Woodlands Hospital on Aug. 18, 2021, in Houston, Texas. Brandon Bell/Getty Images
Medical debt can stymie communities’ economic mobility as unpaid hospital bills chip away at public dollars. That’s why local governments are looking to forgive residents’ medical debt, which experts say can be especially helpful for rural areas.
You're reading Route Fifty's Public Finance Update. To get the latest on state and local budgets, taxes and other financial matters, you can subscribe here to get this update in your inbox twice each month. You can find a full archive of these newsletters here.
Across the country, local governments are starting the new year with bold resolutions aimed at improving residents’ health and addressing economic disparities and inequities. To put their goals into practice, some cities and counties are using federal pandemic-era funds to cancel residents’ medical debt in a bid to enhance economic prospects for both individuals and communities.
The city of St. Paul, Minnesota, for instance, began 2024 with the goal of eliminating more than $100 million of residents’ medical debt.
St. Paul is partnering with the nonprofit RIP Medical Debt to purchase and forgive around 43,000 residents’ medical debt from four private health care systems in the area. Under an agreement, the program partners—Allina Health, Children’s Minnesota, HealthPartners and MN Health Fairview—will share patient medical debt data with the city to identify which individuals have overdue bills that the city and RIP Medical Debt can cover, said Muneer Karcher-Ramos, director of the city’s Office of Financial Empowerment.
RIP Medical Debt usually uses donations to finance its medical debt erasure efforts, but by partnering with St. Paul, the organizations are leveraging the city’s one-time investment of $1.1 million from federal American Rescue Plan Act funds to purchase and forgive medical debt on residents’ behalf.
To qualify for the service, residents must have an income between 0% and up to 400% of the federal poverty guideline or have medical debt that represents at least 5% of their annual household income.
The cost of lingering medical debt often falls on taxpayers, creating a liability of public dollars, said St. Paul Mayor Melvin Carter. Purchasing medical debt is “done every single day in the private sector … for pennies on the dollar. The only difference really is that … our plan is to wipe that slate clean so that it becomes a direct benefit to the residents of our city.”
Residents “don't have to sign up for anything, they don’t have to register, they don't have to enroll,” Karcher-Ramos said. They’ll receive a “surprise letter in the mail to know that their medical debt has been wiped free.”
Using ARPA funds to erase medical debt is an “innovative and creative model … that spans both the health care space but also the socioeconomic and environmental factors that really drive health for individuals and for communities,” said Lori Tremmel Freeman, CEO of the National Association of County and City Health Officials. “As [local] governments are looking for ways to address health inequities and disparities, this … will be interesting to watch in terms of outcomes and what actually happened to the individuals who were relieved of this debt and whether that can be tied or correlated with other types of health outcomes or other types of economic outcomes.”
Almost 100 million Americans are just scraping by because of overdue medical bills, and “anything that brings economic instability to a family or household creates a number of factors that actually impact [individuals’] health,” Freeman said. Medical debt, for instance, can deter people from seeking treatment or preventative care because they can’t afford more doctor bills. Insurmountable bills can prevent individuals from building wealth, securing loans and even obtaining employment, limiting their economic mobility.
Local governments in rural counties can especially benefit from cancelling residents’ medical debt, Freeman said. Rural jurisdictions are more likely to have health-related disparities than urban areas, such as poorer health overall, more risky behaviors such as substance use and less access to health services. Plus, rural residents tend to be older and sicker than urban dwellers—creating a perfect storm for racking up medical debt.
And considering that hundreds of rural hospitals across the country are at risk of closing, “you can likely conclude that medical costs could potentially be more burdensome in rural areas,” Freeman said. Eliminating medical debt for rural residents could greatly impact the health and financial outcomes of rural communities.
In the Appalachian region, for instance, more than $1 billion of medical debt has been erased for more than 770,000 individuals with the help of RIP Medical Debt since 2019. Eliminating medical debt can help ease residents’ other health-related costs such as traveling to a specialist, said the organization’s CEO Allison Sesso.
Plus, hospitals “get a little bit of money to support their systems” when they partner with debt-relief organizations, Sesso said. The money received under medical debt programs may not be enough to completely save their bottom lines, but “every penny counts.”
Elsewhere, Oakland County, Michigan, is also partnering with RIP Medical Debt to turn $2 million of ARPA funds into $200 million of erased medical debt for 80,000 county residents. According to officials, the average amount of medical debt in the community is $2,500 per household. And in Clark County, Nevada, where more than 17% of residents are impacted by medical debt, $2.7 million of debt was relieved for residents late last year.
Ultimately, canceling medical debt is “a bittersweet pill to swallow,” Freeman said, because it means governments continue to focus on health care, but more attention and investment needs to go toward prevention—not just treatment.
Investing in preventative public health programs “saves more money in the long run—[more] than attempting to correct the issue of relieving debt from treating chronic illness and disease,” she said.






