With Vaccine Approval Imminent, States Ready Plans to Give People Their Shots
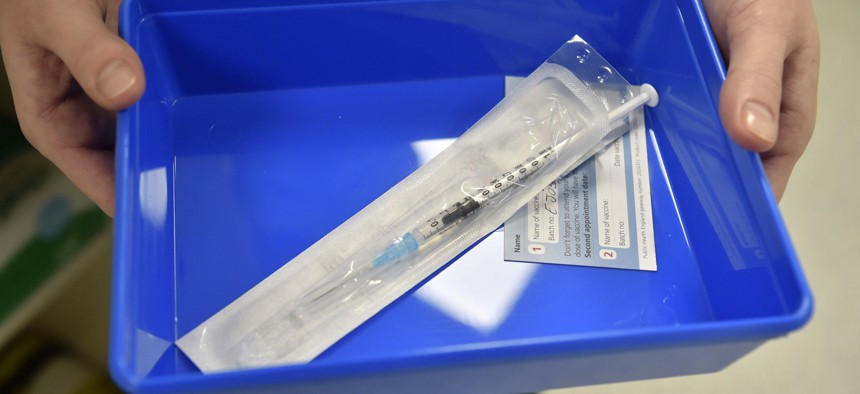
The Pfizer-BioNTech COVID-19 vaccine at a vaccination centre in Cardiff, Wales, Tuesday Dec. 8, 2020. The United Kingdom is beginning its vaccination campaign this week. Ben Birchall/Pool via AP
The federal government could approve and begin distributing vaccines to protect against Covid-19 as soon as next week.
The largest mass vaccination campaign ever attempted in the United States is expected to get underway in the coming days and states are hurriedly finalizing plans that detail how they will receive, store and administer initial doses of the coronavirus vaccine.
Officials are prepared to begin distributing vaccines as early as next week, with the Trump administration expected to distribute roughly 20 million doses by the end of the year. As many as 6 million doses could be sent out to states the first week after vaccine authorization, White House officials have estimated.
The number of vaccine doses the federal government has told states they will receive has fluctuated in recent days as manufacturers adjust production estimates, state leaders said this week. As of Tuesday, Minnesota is expecting 46,000 vaccine doses from Pfizer in the first week and 94,000 doses from Moderna in the second week, said Gov. Tim Walz during a Tuesday press conference on the state’s distribution plan.
“We know we are not going to be able to give as much vaccine that is needed, even for those high priority populations in the first couple of weeks,” said Minnesota Department of Health Commissioner Jan Malcolm.
Minnesota will embrace a hub-and-spoke model of distribution, with the initial batch of vaccines sent to key hospitals and then distributed to smaller health clinics from there as needed, Walz said. Because the Pfizer vaccine must be kept at ultra-cold temperature to remain viable—minus 70 degrees Celsius—the state has also done trial transportation runs to ensure the shipping containers will be cold enough throughout transit to distribution points, Walz said.
The number of vaccines initially available may fluctuate, but “the plan itself is solid,” he said.
While the initial wave of vaccines is destined for frontline health care workers and people in long-term care facilities like nursing homes, states decide which groups will receive certain shares of the vaccine and how the vaccines will be distributed across their jurisdictions.
The vaccines will be distributed to states on a modified per capita base that takes into account the population of frontline medical workers, nursing home residents, first responders, and people with underlying health conditions, a senior Trump administration official said during a press briefing this week.
States have developed their own plans to administer and distribute vaccines based on local circumstances. The White House held its own Operation Warp Speed vaccine summit on Tuesday, at which governors from Louisiana, Tennessee, Texas, and Florida discussed their distribution plans.
Texas Gov. Greg Abbott said the state now has 7,200 health care providers signed up to administer the vaccine once it is available.
In Florida, five designated hospitals in Orlando, Miami, Tampa, Jacksonville and Hollywood will receive the first round of vaccines, which will be provided to health care workers employed at those hospitals and those who work elsewhere.
Similar to Minnesota’s model, Illinois will distribute vaccines to the state’s 10 regional hospital coordinating centers, but will transfer to county health departments based on the highest death rates per capita.
Some public health officials worry that the logistics of vaccine distribution will be more complicated and take longer than many would like to see, particularly in rural areas. In addition, it still remains unclear how quickly the vaccine will become available. While the Food and Drug Administration so far has given a positive review of the Pfizer vaccine, news outlets this week reported that the Trump administration passed on an opportunity to quickly secure more than 100 million doses, raising questions about how long the country will have to wait for more of this particular vaccine to become available.
In Maryland, Gov. Larry Hogan said Tuesday that the state expects to receive an initial batch of 155,000 doses of vaccines. A second dose of the vaccine is needed to be effective and Hogan said the federal government plans to hold back enough doses so that the final shot can be provided several weeks later.
More than 2,300 Covid-19 deaths in Maryland occurred in nursing homes or assisted living facilities, and frontline health care workers as well as nursing home residents and staff will be the two targets for the initial round of vaccinations. Once most of the initial target population have gotten or been offered the vaccine, Maryland will move into its second phase of vaccinations with the priority going to workers who are critical to schools, transit and other critical infrastructure.
Some people may not want to be vaccinated, and public health officials plan to work with local leaders on public education and outreach efforts, said Dr. Bryan Mroz, assistant secretary of the Maryland Department of Health.
“We want to collaborate with trusted community leaders and community voices to understand community hesitancy,” Mroz said. “We will communicate what we know and what we don’t know.”
Andrea Noble is a staff correspondent with Route Fifty.
NEXT STORY: As the Pandemic Rages, the U.S. Could Use a Little Bit More 'Samfundssind'





