How States Are Evaluating Medicaid Eligibility for Millions
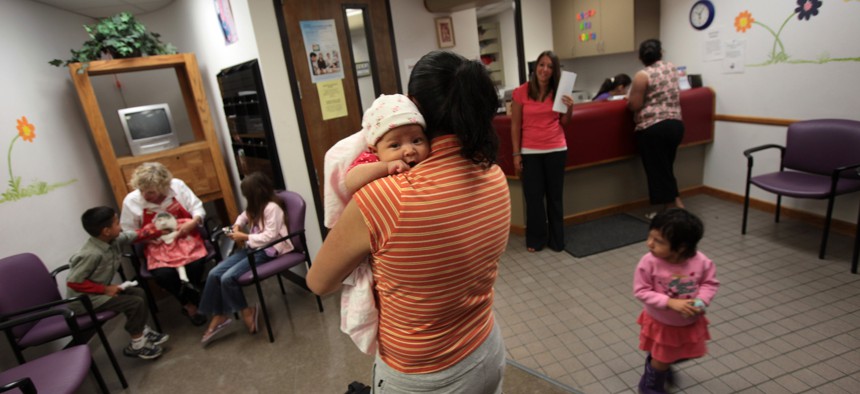
States must evaluate over the next 14 months the eligibility of the roughly 93 million low-income people are on Medicaid. John Moore via Getty Images
States have 14 months to reexamine the eligibility of the roughly 93 million people on Medicaid. The approaches and timelines for review vary widely state by state.
Faced with the herculean task of checking whether all of the nation’s roughly 93 million low-income people on Medicaid still qualify for coverage over the next 14 months, states are taking widely different approaches to the amount of time they’ll take, how they’ll verify information and the methods they’ll use to warn people of possible or actual changes to their coverage.
“It really is a big task and it's a big task for every state because we're all in the same boat,” said Heidi Capriotti, public information officer for the Arizona Health Care Cost Containment System, which provides Medicaid for 2.5 million people in the state.
States were barred from dropping people’s coverage during the pandemic, but that’s ended now. Congress discontinued the restriction in the $1.7 trillion omnibus spending bill it passed in December, allowing states to remove those who do not qualify from the rolls on April 1. States have 14 months to make sure everyone in the program is eligible.
Each state is working at a different pace, according to a survey released last week of state Medicaid agencies conducted in January by the Kaiser Family Foundation and Georgetown University’s Center for Children and Families.
Interviews with health department officials in numerous states, along with the Kaiser survey, reveal that some never stopped tracking eligibility for Medicaid and are prepared to begin culling their rolls. Meanwhile, other states say they need time to verify information and to reach recipients in order to avoid dropping people based on erroneous information.
About half the states began telling people they would have to reapply for Medicaid before April. People in those states who don’t qualify will lose their coverage this month. The other half of the nation, and the District of Columbia, have waited to begin telling people that they have to reenroll until this month. People in those states are not expected to be dropped from the program before June.
States are also prioritizing who to reexamine for eligibility first.
For instance, Oklahoma, which is planning to examine the eligibility of 18,934 people in April, said it is prioritizing people who would be least at risk of being harmed if they were to lose coverage, including those without children younger than five, those who have not filed any recent medical claims, or residents who earn more than twice the federal poverty rate and have coverage because the state expanded Medicaid in 2021.
In some states, those being prioritized first are people hitting the anniversary of when they first signed up for the program. Other states, like Arkansas and Arizona, will reexamine those who are no longer eligible for Medicaid because of their earnings or residency.
The timelines for decisions vary by state as well. Most states report that they plan to take between a year and the full 14 months allowed to complete the effort, according to the survey. Five states—Arkansas, Montana, New Hampshire, Oklahoma and South Dakota—are planning to finish in as little as nine months.
Asked why Oklahoma is trying to finish in nine months, Emily Long, a spokeswoman for the Oklahoma Health Care Authority, said the tight time frame meets the Centers for Medicare & Medicaid Services directive that not more than 1 in 9 people on Medicaid be removed a month. She added that her state is positioned to move quickly because its automated system makes it easy to compare data collected by different programs.
Those deemed ineligible in Oklahoma will get notices by mail, email, text and phone that they have to reapply. After making a “good faith effort” to reach them, as required by Congress, those deemed ineligible for Medicaid will be dropped.
“We have full confidence that our error rate will remain low,” Long said.
Most notably, Arkansas’ legislature directed its state Medicaid office to cull the list within six months, or about twice as quickly as most states.
“Unwinding the continuous enrollment condition will be one of the largest and most complex efforts for state Medicaid programs since the implementation of the Affordable Care Act almost a decade ago,” the state’s Department of Human Services said in its plan for the effort. “States, including Arkansas, will face challenges during the unwinding, particularly related to workload and staffing.”
Much will be on the line in the month ahead, said Bradley Corallo, a senior policy analyst with Kaiser’s program on Medicaid and the uninsured. About 15 million people are expected to lose their Medicaid coverage, according to an estimate by the U.S. Department of Health and Human Services. But most concerning is that, according to the estimate, about 6.8 million of those who will lose coverage are expected to be wrongly booted from Medicaid even though they qualify for the program.
Another concern, Corallo said, is how well states will be able to reach people to let them know they have to reenroll.
“Housing instability was a problem [during the pandemic],” he said. “A lot of people were moving, especially among the low-income population. So we're really concerned about states trying to reach out to these enrollees to verify information like their income.”
That some states are trying to finish much earlier than others is “definitely a big concern of ours,” said Farah Erzouki, a senior health care policy analyst for the progressive Center on Budget and Policy Priorities.
Several factors influence the pace states are taking, including their situation during the pandemic, according to Medicaid officials in Arizona and Missouri.
Arizona, which began sending out renewal notices in February, was prepared to begin the process, Capriotti said, in part because the state continuously monitored Medicaid eligibility based on income since it wasn't sure when the pandemic and restrictions on assistance would end.
“Arizona never stopped its renewal process. We only stopped our disenrollment process,” Capriotti said. “We continued to run renewals throughout the last three years. That gave us a little bit of insight as to where people might stand once we turned renewal processes back on.”
Because of that, the state has identified thousands of people they think might be ineligible. If they, or any of the others on MedicIS are deemed to no longer be eligible for the program, the state will refer them to get health care coverage through other ways, including subsidized insurance through the Affordable Care Act marketplaces, Capriotti said.
Missouri, though, is starting a little later in reexamining the 1.5 million people on Medicaid. Rather than monitor eligibility during the pandemic, said Kim Evans, director of family support for the state’s Department of Social Services, her team focused on adding about 370,000 people to the program when the rules changed to include those with higher incomes.
“We were trying to get through the backlog of applications,” she said. “So we just didn't focus on the annual renewals because we knew we had to get these applications processed.”
The state is starting this month by comparing the information of the people on Medicaid with other information it has from, for example, the food stamp program. “By the end of the month, we will know how many annual renewals we will have to send out,” Evans said.
While all states have the ability to compare databases in order to speed the process, some say taking the full amount of time allotted gives Medicaid recipients more time to respond to requests for information.
“There’s 2.5 million people, so dividing that over the course of 12 months, makes the workload manageable,” said Arizona’s Capriotti. “And it makes it so that we have time to get responses from those people who have not responded to our requests for information.”
Taking a full year would give the state more time to track down people before taking away their health coverage, said Bob Wheaton, a spokesman for the Michigan Department of Health and Human Services.
The survey, for instance, asked states what they plan to do if their mailings telling families they must reapply or lose their coverage are returned. Two states, California and Maryland, said in the survey that they planned to follow up with texts, emails and with phone calls to make sure people know they have to reapply. Other states, including Michigan and Arizona, told Route Fifty that they plan to do the same.
Another 12 said they also planned to email if they couldn’t reach people by phone and nine states said that in addition to calling they’d try to text people, according to the survey.
Missouri, like many states, also said they are working to get contact information from managed care providers or have asked them to tell Medicaid patients to re-enroll. Evans also said Missouri will be launching an online portal in May that will let people on Medicaid check their status.
Staff vacancies are also slowing the process. The survey reports that 16 states say more than 10% of their Medicaid positions are vacant. Thirteen states said they have vacancies for more than 10% of their call center positions. West Virginia Department of Health and Human Resources will take the full year allotted to reduce worker fatigue and accommodate staffing limitations.
Kery Murakami is a senior reporter for Route Fifty, covering Congress and federal policy. He can be reached at kmurakami@govexec.com.
NEXT STORY: Fight Between States Could Determine Fate of Abortion Pills






